When a patient with severe respiratory symptoms arrived in Brazil’s public health system during the SARS-CoV-2 pandemic, a chain of work followed. A nurse collected the sample. A public laboratory processed it. A bioinformatics team assembled and checked the viral genome. All of this was funded through a constrained public budget and carried out by professionals working under pressure in an under‑resourced setting.
The sequence was uploaded to a global database within hours, in the expectation that it would strengthen surveillance, support variant detection and contribute to a coordinated global response, which included equitable access to the vaccines, diagnostic tests and therapeutics.
What happened next is the problem.
Once the sequence entered the international system, however, there was no mechanism to record its downstream use, such as who downloaded it, which products it contributed to, or whether any benefit would return to the health system and communities that made it possible. The data left. The benefits did not follow. This experience is not unique to Brazil, it happened to Namibia, South Africa, and countless other countries, and it reflects a broader reality for many developing countries that contribute pathogen data to global platforms.
The WHO Pandemic Agreement, adopted in May 2025, was meant to change this. Article 12 establishes a Pathogen Access and Benefit-Sharing (PABS) system on an "equal footing" principle: those who access pathogen data carry obligations matching those who provide it. Whether that principle means anything depends on one unresolved question in the ongoing PABS Annex negotiations: can users be identified, their use traced, and their obligations enforced? Under proposals currently advanced by several developed countries, the answer is no.
A benefit-sharing system requires, at minimum, the capacity to identify who has used covered data, for what purpose, and with what outcomes. Without user registration, none of these conditions can be met. A sequence deposited under an anonymous-access model can be downloaded by a public health institute, a pharmaceutical company, a biotechnology firm, or an academic laboratory, with no record of the transaction. There is then no mechanism to determine which sequences contributed to which products, no basis for invoking benefit-sharing obligations, and no means of monitoring compliance. The equal footing principle of Article 12 collapses at the point of data access.
One concern raised by developed countries in the PABS Annex negotiations is that requiring registration or accepting data‑access terms could slow research or undermine open access. The claim that registration is incompatible with open science is not supported by evidence. Many widely used repositories already require user registration, identity verification, and data-access agreements, while serving tens of thousands of researchers in nearly all countries. Controlled-access genomic repositories and trusted research environments have demonstrated that it is possible to combine rapid data access with robust governance. Researchers routinely log into databases, accept terms of use and still conduct time‑sensitive, large‑scale analyses.
A second concern is that registration and data-access agreements could threaten interoperability or machine‑to‑machine data exchange. This claim is similarly unsupported. Interoperability is a function of shared formats, metadata standards, and application programming interfaces, not of user anonymity. Contemporary information systems routinely authenticate both human users and automated agents while maintaining highly interoperable architectures. This is true in health, finance and other data‑intensive sectors, and there is no inherent reason pathogen databases should be different.
A third line of argument invokes the UNESCO Recommendation on Open Science. However, although that instrument addresses open access to data, it also states explicitly that data should not be unfairly or inequitably extracted in the name of openness. It does not override sovereign rights under the Convention on Biological Diversity, and it was not designed to prevent countries from attaching reasonable conditions to the use of their biological resources. In practice, open science encompasses more than the absence of conditions. It addresses who can participate in knowledge production, who can use the outputs and how benefits are distributed. Selectively citing UNESCO to argue against any access conditions undermines the very equity principles the Recommendation was designed to advance.
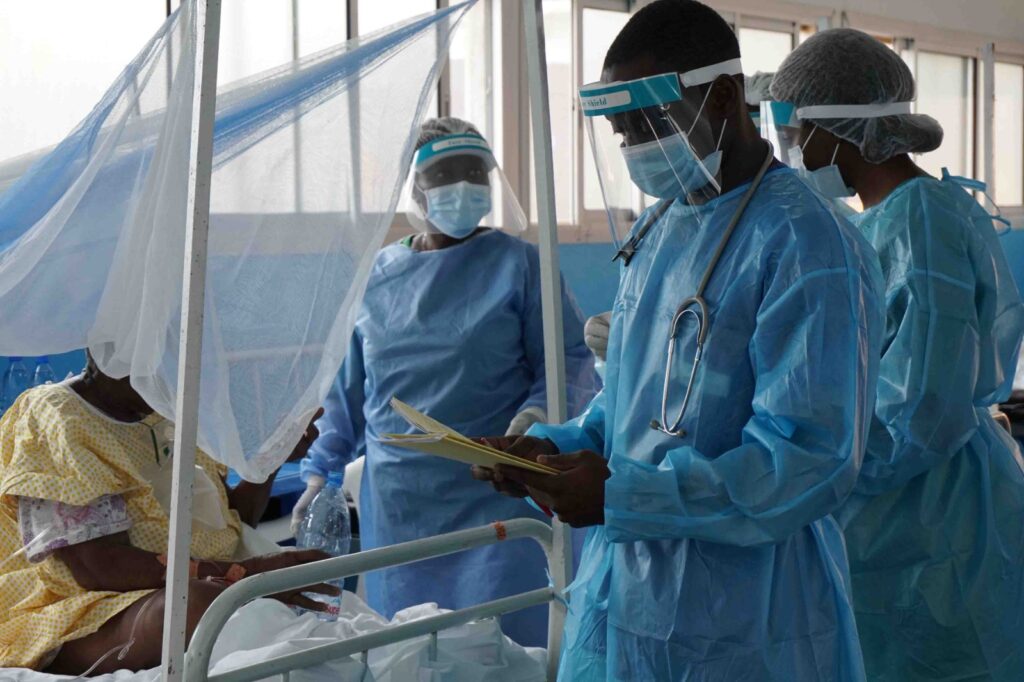
Healthcare workers attend to a patient in a hospital ward in Cameroon during the COVID-19 pandemic in 2021. Credit: Vanessa Fodjo/MSF
There is a historical precedent worth noting. The Pandemic Influenza Preparedness (PIP) Framework, adopted after Indonesia withheld H5N1 samples in 2006 over inequitable vaccine access, was the first attempt to link pathogen sharing with benefit-sharing. Independent analysis has consistently found that, while it effectively secured access to virus samples, it failed to reliably deliver benefits to provider countries, in part because the mechanisms linking use to obligation were too weak. PABS is being negotiated in the shadow of that failure. Reproducing the same structural gap would be a conscious choice, not an oversight.
The COVID-19 pandemic illustrated the consequences at scale. By late 2021, developed countries had administered more than one vaccine dose per person on average; developing countries, many of which had contributed sequence data to the global response, had administered fewer than four doses per hundred people.
It is worth being precise about what is being proposed, because it is frequently mischaracterized. Developing countries are not seeking complex bilateral contracts for every data transaction. This includes academic users. Publicly funded laboratories routinely generate findings used downstream in commercial development, and excluding them from any accountability framework breaks the chain of traceability between public data and private product. What is being asked for is a standardized, low-friction framework that applies to all users: registration with verified institutional affiliation, a standard data-access agreement setting out transparency obligations and benefit-sharing participation, and basic monitoring capacity to track how PABS-tagged data are used and in which sectors.
These are not novel conditions. Within the European Union, material transfer agreements and data-access agreements govern the exchange of biological materials and sensitive data as standard practice. Nagoya Protocol implementing regulations define mutually agreed terms as contractual arrangements for benefit-sharing. The same governance norms that developed countries apply domestically to protect their own genomic data are precisely what developing countries are asking to be extended to data originating from their hospitals, laboratories, and communities.
A bloc of approximately a hundred developing countries has consistently called for mandatory benefit-sharing, including guaranteed access to vaccines, therapeutics, and diagnostics, as a condition of rapid pathogen data sharing. That position reflects a shared assessment, informed by the COVID-19 experience, of what a system without enforceable traceability produces in practice.
The March 23–28 session of the WHO Intergovernmental Working Group is the last scheduled round before the PABS Annex goes to the World Health Assembly. Existing platforms demonstrate that open science and accountable data governance are compatible—the question is whether negotiators will build that compatibility into the Annex. User registration, data-access agreements, and monitoring capacity are not obstacles to a functional PABS system. They are what make one possible.
AIDS Healthcare Foundation (AHF)

