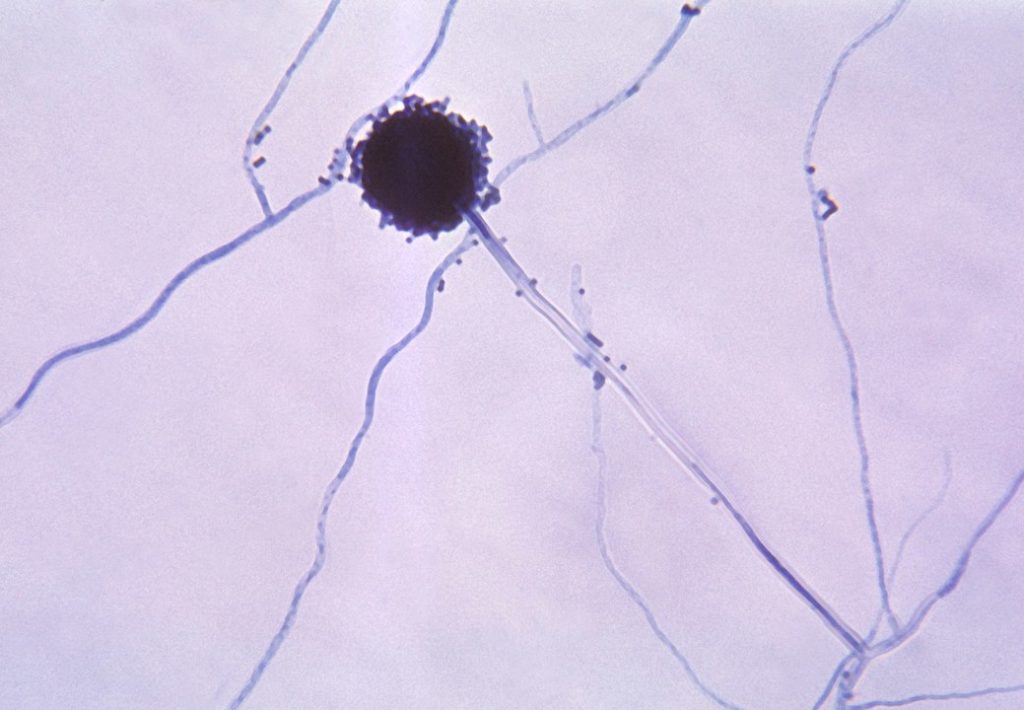
One in six patients admitted to intensive care as a result of a serious Covid-19 infection were also suffering from a fungal infection, and half of those patients died as a result, according to international research.
The figures are not definitive, but the overall trend suggests that between 3,750 and 4,000 patients in Belgium may have been infected with the fungus Aspergillus, which is thought to have aggravated the symptoms of Covid and affected the outcome.
Aspergillus is in fact a family of fungi, discovered in 1729 by an Italian priest-biologist, who named it after the holy water sprinkler used in church (aspergillum in Latin) because of its shape.
Some species are used in commercial and medical applications; others are pathogenic, and can cause diseases in humans as well as crops.
The disease aspergillosis caused by the fungus may easily go unnoticed in Covid patients, particularly those who are serious enough to be admitted to ICU and require a ventilator to breathe. Because the fungus has similar symptoms, the only way it can be detected is by carrying out a specific test.
“Much depends on the alertness of the attending physician,” Professor Katrien Lagrou of Leuven university hospital, who specialises in life-threatening fungal diseases, told the VRT.
“The doctor should think about testing for fungi, but not everyone has that reflex. Fungal infections used to be one of the most missed diagnoses,” she said.
“We used to rarely look for fungal infections,” confirms Yves Debaveye, a member of he ICU staff at the hospital.
"Often the diagnosis was only made after the patient's death, at an autopsy. Fortunately, that has improved in recent years."
Aspergillus is common in our environment – in the soil, in compost, buildings materials and so on. We inhale an estimated few hundred spores a day, but our bodies can fight them off. In people with a compromised immune system, however – such as someone already battling a viral infection like Covid – the fungus gets a chance to take hold, and unless steps are taken, the effect can be disastrous.
The treatment of choice in such cases is voriconazole, a drug made up of azoles – compounds used to combat fungal infections in humans and crops. The trouble is, Aspergillus is becoming more resistant to azoles, in the same way that bacteria are becoming more resistant to antibiotics.
The Leuven hospital tests each species of Aspergillus for resistance, and its numbers show that 7% of those patients who have an infection are infected by a resistant strain.
Scientists are now working to find out where the hot-spots of resistance are in Belgium, starting with places where azoles are in widespread use, such as agriculture and horticulture.
"We definitely need to map that problem well," said Prof. Lagrou. "Aspergillus is everywhere in the environment. There is a risk that those resistant strains will spread further. And that they can infect more people."