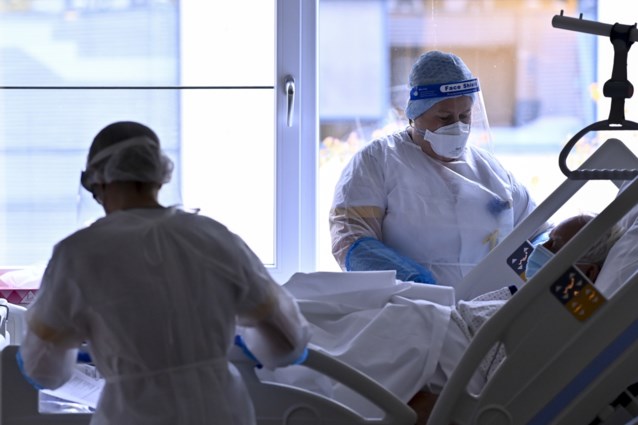
Why do some people who become infected with the SARS-CoV-2 virus suffer relatively few ill-effects, while many other become very sick and even die?
A research study led by a team from the university of Edinburgh may have provided at least part of the answer: genetics.
The study looked at the genome of more than 2,000 people in the United Kingdom who has suffered serious symptoms of Covid-19, compared those profiles with about the same number of health people, and detected eight genetic sequences common to the Covid patients.
Looking more closely, they narrowed the difference down to two genes, TYK2 and CCR2, which have a role in the body’s inflammatory response to infection.
One of the principal symptoms of Covid-19 infection, and a leading cause of death, is severe respiratory problems. Even patients who do not die often have to go through intensive care (ICU) and time spent on a respirator.
“We have shown that people who produce more of the TYK2 protein are more at risk for [severe effects from] Covid,” said lead researcher Dr. Kenneth Baillie, at an online press conference. “However, there is a drug on the market that inhibits it,” he said.
In fact there is a series of drugs on the market which inhibit the action of TYK2, known as JAK inhibitors, which are mainly used to treat rheumatoid arthritis – an autoimmune disorder – and are being investigated for use in the treatment of conditions as diverse as psoriasis, atopic dermatitis, alopecia, ulcerative colitis and vitiligo.
Also, Dr. Baillie said, trials are underway to look at the effect of using synthetic antibodies to combat the CCR2 protein.
The Edinburgh research involved 210 ICUs across the country providing data on patients, as well as more than 1,400 research staff working on the project itself.
“This demonstrates the beauty of genetics for drug target discovery,” Dr. Baillie said. “Faced with a new disease, that we didn't understand at all, we can look across the entire code that makes our immune system, to find the exact points we need to target with drugs, in order to save lives.”
However, while the research offers a useful path for further investigation, it is not the road to a cure.
“Of course, as we say in the paper, we can't know that any of these drug predictions will actually work until we do large-scale, randomised clinical trials.”
The study is published in the latest issue of the journal Nature Research.
Alan Hope
The Brussels Times