Scenarios presented to the government showed that hospitals could run out of beds in intensive care units (ICU) if the infection rate doesn't decrease in Belgium.
Hospitals across the country must now reserve 50% of ICU beds for Covid-19 patients, resulting in the postponement of other care, and if the ongoing fourth wave doesn't slow down in the coming weeks, the situation could become much worse and remain dire until February 2022.
Based on calculations made by the UAntwerpen and UHasselt's SIMID consortium, five scenarios for the coming weeks were presented to the Consultative Committee on Wednesday, including a best-case and worst-case.
In the worst-case scenario (the yellow dotted line on the graph below) - which assumes the current reproduction rate (Rt) of 1.12 continues to increase until December 2021 - the peak ICU load will reach around 850 at the start of December.
Eventually, more than 1,200 beds would be occupied by Covid-19 patients at the peak, meaning hospitals could face running out of ICU beds and it would take until February to gradually decrease to a level below 500 ICU beds.
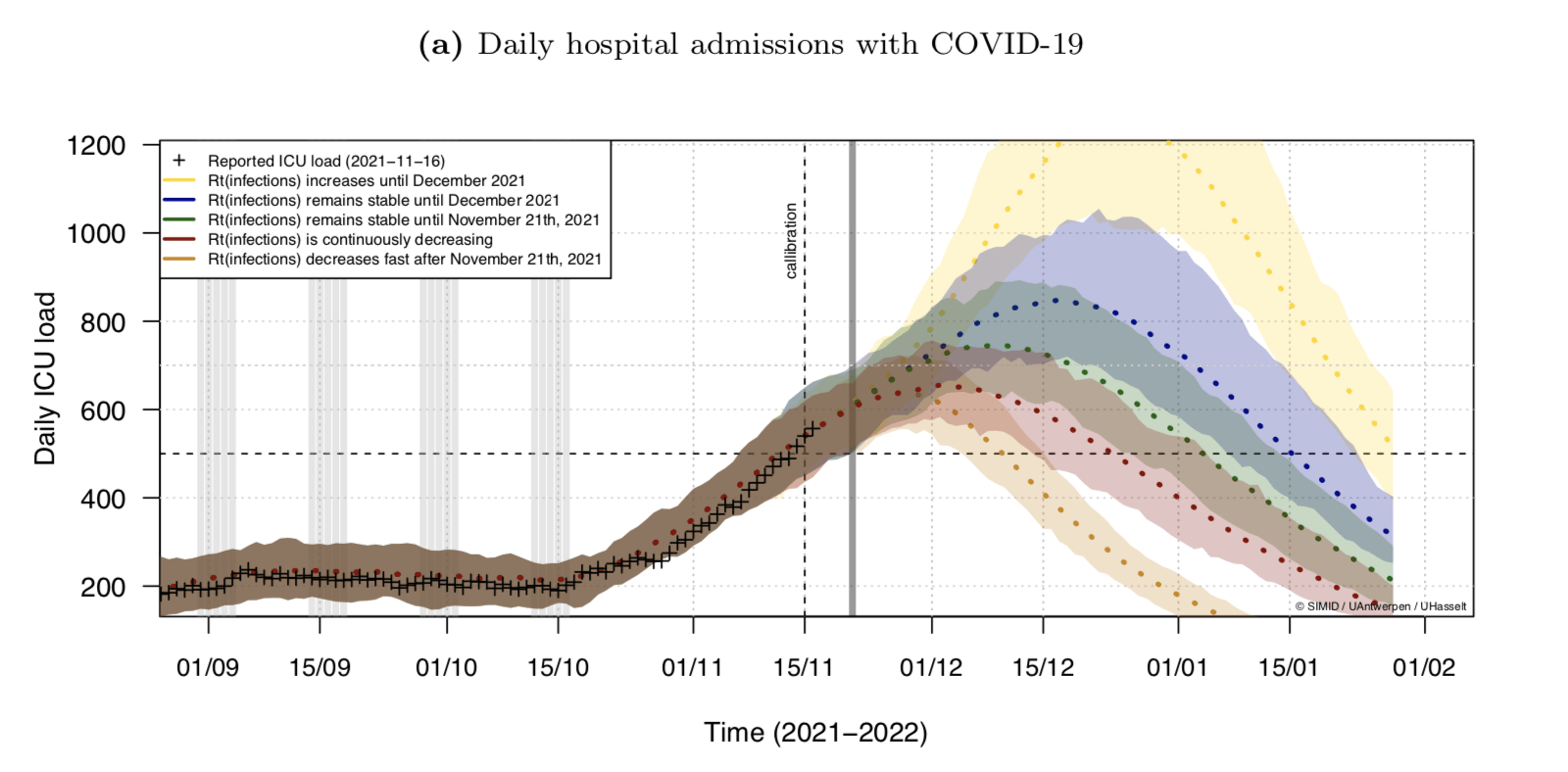
The five predicted scenarios. Credit: SIMID
Another scenario (coloured blue) that assumes infections remain stable until December would see the number of Covid-19 patients in ICU peak at 850 by midway through the month.
If the situation remains stable until 21 November (green), a peak ICU occupancy of around 750 beds could be reached in December 2021.
If the slowly-decreasing infection rate continues its trend as a result of the new measures announced by the government on Wednesday, the ICU occupancy is still expected to reach 650 by the start of December (red), but a quicker decrease in the infection rate (beige) could see a rapid decline in the ICU load after this peak, decreasing to less than 500 beds by the second week of December.
Most experts, including virologist Steven Van Gucht (Sciensano), predict the latter two scenarios aren’t realistic, and that the green scenario is most likely to happen, according to reports from De Standaard.
This would still mean postponing non-urgent care until at least February, as more than 300 Covid-19 patients in ICU result in the rescheduling of treatments.
Adding salt to the wound
Any of the scenarios are alarming when almost 200 out of the almost 2,000 available ICU beds across Belgium are already unavailable as a result of staff shortages, as healthcare personnel cancel shifts either because they themselves have contracted Covid-19 or another illness, or because they have to go into quarantine following close contacts with an infected person.
While health care workers are now being invited to receive their third dose of a coronavirus vaccine, the effects of this will only be seen two weeks following the administering of the shot.
Related News
- 'Too little, too late': experts divided on Belgium's latest measures
- 'Bare minimum measures, or complete lockdown,' says health minister
Normally, ICU beds in Belgium are occupied by 1,400 to 1,500 patients receiving various treatments. But as of Thursday, there are almost 580 Covid-19 patients taking up those beds instead, with the infection rate currently at one of the highest levels recorded since the start of the coronavirus crisis.
According to the ICU-prediction model made by the SIMID group, over 740 patients will be in ICU on 26 November, and it's possible 1,000 ICU beds will be needed for Covid-19 patients by the beginning of December if hospitalisations and intensive care unit admissions increase at the current pace.
The figures are based on the current number of infections that have already been recorded and the increasing trend of new cases, as "infections as a result of social interactions drive the projected hospital burden," highlighting that people's close contact behaviour will have a big impact on these figures.
